The options for orthotic design and materials, like footwear, depend on the condition of the plantar skin integrity (scar tissue), foot deformity, and patient activity level. The purpose of a molded orthotic is to increase the surface area in contact with the foot and distribute the forces created by walking more evenly across the foot. The orthotic reduces focal areas of pressure that can lead to ulceration. A wide selection of materials is available to achieve a balance or proper gait mechanics and pressure reduction.
Creating orthotics for someone without sensation requires added attention to assure a safe fit. In most cases, the patient will not be able to provide accurate verbal feedback on the feel and fit of the orthotic. You will need to perform frequent skin inspections to ensure the orthotic is not producing irritation and skin breakdown.
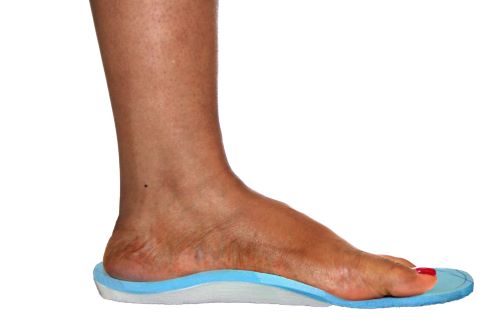
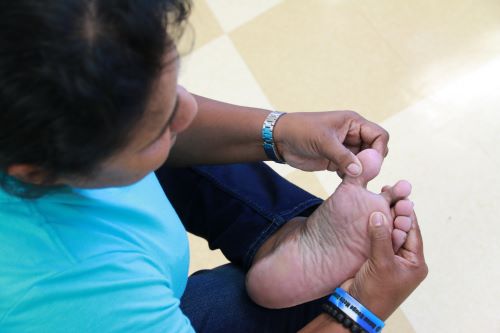
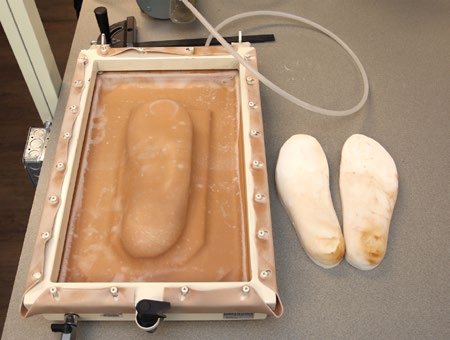
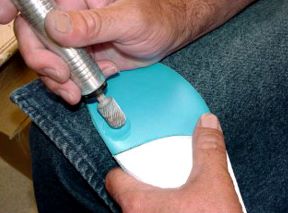
Custom orthotics can be created by press molding the material directly to the patient’s foot, by using a vacuum press on a positive model of the patient’s foot, or by using a computer and CAD CAM device. During the fabrication, contours may be added to the orthotic to provide additional pressure relief. Localized pressure relief may also be obtained with a handheld Dremmel tool or grinder.


With every new shoe and custom orthotic, the patient and health care professional should monitor the feet closely for signs of redness, localized temperature increase, callus, swelling, pre-ulceration, or recurrence of a previous ulcer. Immediate attention to signs of pressure will help prevent ulceration.
Appropriate orthotic and footwear selection
Risk Category 0: No loss of protective sensation (can feel the 10-gram monofilament)
Soft non-molded orthotic worn for comfort and function. Most standard orthotics that come with the shoe are appropriate for this risk category. The patient can use any footwear.

Risk Category 1: Loss of protective sensation (does not feel the 10-gram monofilament), no deformity, callus or signs of abnormal pressure.
Soft molded or non-molded orthotics would be appropriate. The level of customization would depend on the evaluation of the patient’s future risk, type of job, and activity level. Patient may require extra depth footwear.


Risk Category 2: Loss of protective sensation (does not feel the 10-gram monofilament), foot deformity, presence of callus or high-pressure area.
Soft molded orthotic with modifications to relieve pressure over a bony prominence or other high-pressure area. The level of customization would depend on the evaluation of a patient’s future risk, type of job, and activity level. The patient would require extra-depth footwear. Rigid rocker soles or other footwear modifications may be necessary based on the deformity.


Risk Category 3: History of plantar ulceration or Charcot deformity or neuropathic fracture.
Soft molded orthotic with modifications to relieve pressure over the callus or other high-pressure area. The level of customization would depend on the evaluation of the patient’s future risk, type of job, and activity level. The patient would require extra-depth footwear. Rigid rocker soles or other footwear modifications will be necessary based on the deformity. Extra wide or custom shape footwear (wide shank) to accommodate Charcot deformity should be considered if warranted.
